Empathy is … communicating that incredibly healing message of you’re not alone (Brene Brown)
In recent years I have been a manager and leader in health care provision and in my last post as chief executive of a children’s hospice and through my senior management team I set the boundaries of care including the criteria for acceptance into the service and the quality of the provision for the benefit of the users. I had oversight of the service ensuring it was meeting the needs of the user and the standards set out by the Care Quality Commission (CQC). Whilst the service was small in comparison to any NHS Service provider nevertheless it operated in similar ways. So now I am a recipient of care and the table has been turned and it has been illuminating – from the many discussions with care assistants whilst in the shower, challenging the stroke consultant about goal setting, recognising the need for coordination of services available from community services, which I have found very difficult to navigate, insisting on physiotherapy following my hip replacement (when none was forthcoming), to the attitude of some staff towards me and other patients. So, there is a lot to recount. It has been challenging for me as I was the one who led and provided the care service and now the balance of power has been turned and I am the one who has to receive it.
I have had care and support offered by a myriad of health and social care professionals, the list is long and certainly tricky to navigate. This is compounded by endless appointments often in Norwich which is an hour’s drive away. It is tiring and tiresome, tedious in the extreme when all I wish for is to have my life back to enjoy retirement! Whilst it is amazing to have all this support, mainly state provision, the reality of loss remains. The list of professionals includes:
- Stroke consultant
- Consultant Neurologist
- Epilepsy nurse specialist
- Nurses including those on the ward(s)
- Community nurse
- Health care assistants
- Physiotherapists (private and NHS – including two different organisations probably outsourced by the NHS)
- Occupational therapists
- General practitioners (GPs)
- Speech and language therapist (SALT)
- Psychologist
- Consultant Geriatricians (can you believe it!)
- Mental health service (for cognitive behavioural therapy)
One thing I would suggest to the Clinical Commissioning Group is a designated stroke co-ordinator post (probably a nurse) to help patients certainly after discharge. An excellent person providing such coordination and who has been hugely supportive and helpful is the specialist epilepsy nurse Debbie who has been in touch with both Duncan and me since I started with my epilepsy. She provides advice, regular visits and telephone support as well as liaison with the neurologist to manage my medications which has been crucial.
Whilst in hospital (on 3 occasions) a lot of direct care was provided by health care assistants (or similar titles). Because of their direct contact usually of an intimate nature, this lowers the barrier toward better communication and so often this allows for a full and open discussion. On more than one occasion we had a sing (which lifted my spirits), another a discussion about my sadness and distress, sometimes we spoke about the culture of the ward as well as the training offered focusing on the needs of patients. On more than one occasion I asked the question “so who is the most important person in this building?” Various answers would be given including the manager, doctor until they got it – the patient! I really wanted to add if it was not for the patient there would be no money forthcoming which would mean they would not get paid!! (the wrong emphasis to make perhaps?). I also asked what training they had received about loss and grief in anticipating the need of any stroke patient facing a significant loss and their consequent grief/grieving. I would talk quite freely and openly about how I was feeling.
Here I am being hoisted whilst undergoing rehabilitation


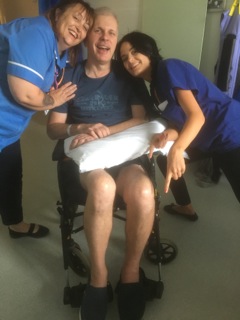
The medical care I received whilst in hospital was excellent and was provided through a stroke consultant team based at the Norfolk and Norwich university Hospital NHS Trust. One of them has been terrific both whilst I was in hospital and in follow up as an outpatient. The quality of his care is in his approach and warmth was very welcome indeed. He has been approachable, and answered questions positively and with reassurance. For example, he explained what had happened when I had my stroke, including the size of it (a massive bleed as big as a fist), that a blood vessel had burst probably caused by high blood pressure over a prolonged period that the recent scans and tests indicated this was unlikely to happen again in the near future (phew!!).
The consultant neurologist has been really helpful in managing my epilepsy, helped by the specialist epilepsy nurse who liaises with him as and when my medication needs to be changed usually after a seizure. I did put him on the spot at my last outpatient appointment asking about my life expectancy following stroke and subsequent epilepsy. I think he was rather taken aback but he did respond to reassure me there should not be any consequence.
Once home and after the early discharge team and first response team discharged me, we were most fortunate to employ a lovely carer who lives just across the road. How good is that!! Sheila (name concealed) and I often have wonderful conversations in the shower and whilst I am being dressed, and despite my initial massive embarrassment about being naked in front of someone the level of conversation has been a very therapeutic experience and Sheila and I talk a lot (not sure if I do most of the talking or she does? Those that know me perhaps know the answer to that one!!). Sheila also does our housework once a week giving Duncan a chance to go out on his own. I of course love the fact that the dust is being dealt with!!
What a blessing she is!
I find a lot of therapeutic care has come through our cats!! (Apologies to those non-cat lovers). They seem to know I have been ill and one in particular lies on my bed and watches me and is quite content to sit close and be stroked whilst I look out of my bedroom window to our wonderful garden. This allows me to rest and reflect. Something I have had to learn to do when I am captive like this.

Barney and Suki my therapeutic friends

Suki little madam!
Richard Rohr a catholic priest and theologian speaks beautifully about the second stage/ second half of life and how this emerges from the first half and is a very different and productive (on another level). I feel I have been catapulted into this stage of life but I find it hard to accept and embrace what this might mean.

Friends and previous colleagues also came to help out
As I sit waiting in the morrisons café (Morrisons? I do apologise but we do not have a Waitrose nearby!). I notice many things one might miss and not appreciate before disability, the kindness of the check-out woman to an elderly customer, the fact the café server is wearing hearing aids within a noisy environment the elderly gentleman in his wheelchair being spoken with by two women who looked like they might be his carers but who kept pinching his chips without asking and the look on his face .The inevitable screaming child (going right through me and my hearing aids!) and mum looking fraught and maybe embarrassed? The café assistant who smiles at you somewhat benevolently perhaps. I feel very conscious about the way some people look at you in a wheelchair or am I being too sensitive? (Do I see myself as someone to be pitied?) So, despite my disability there is a depth and quality to life that can be missed when being busy working and perhaps being in a family juggling many important things, which is how I lived prior to my stroke and which having lost this it is very hard to make the adjustment. I will persevere!

Here I am now my mouth droop has nearly disappeared (but I could do with a better hair cut maybe?)

Hi Peter
A really honest and insightful account of your stroke journey told with humour and candour. Great to see someone sharing their lessons from life for the benefit of others.
God bless you
LikeLike
Dear Darrell – great to hear from you and thank you for reading and responding to my latest blog. I hope to write another one soon so you will be able to see this soon.
Many thanks again and love to you all
Peter xx
LikeLike
Dear Peter, so very sorry to learn about what you’ve been through. Your blog account was very honest and very moving. I wish you all the best as you recover. God bless you.X
(you may remember me when we were teenagers at TRC when I was Catherine Brown)
LikeLiked by 1 person
Dear Catherine, how good of you to get in touch and yes I do remember you. It is great that so many of us from TRC days are in touch. so many memories! What are you doing these days where do you live? Many thanks again. much love Peter xx
LikeLike